Find affordable assisted living facilities detroit. Explore costs, financial aid, and resources for seniors in Detroit.

The Art of Engagement: Exploring Therapies and Amenities in Memory Care
The Art of Engagement: Exploring Therapies and Amenities in Memory Care
Understanding the Growing Need for Specialized Dementia Care
Behavioral memory care is a specialized level of long-term care for individuals living with Alzheimer’s disease, dementia, or other forms of cognitive decline—especially when paired with behavioral health challenges like anxiety, depression, paranoia, or aggression. Unlike traditional memory care, behavioral memory care integrates strategies that support residents’ emotional and behavioral well-being alongside their cognitive and physical health needs.
Key Differences Between Traditional and Behavioral Memory Care:
| Feature | Traditional Memory Care | Behavioral Memory Care |
|---|---|---|
| Focus | Cognitive decline and daily living assistance | Cognitive decline plus behavioral health conditions |
| Staff Training | Basic dementia care training | Specialized training in de-escalation, behavioral triggers, and mental health support |
| Resident Profile | Individuals with memory impairment | Individuals with memory impairment and co-occurring conditions (anxiety, PTSD, depression, aggression) |
| Approach | Routine-based care and supervision | Person-centered behavioral interventions and root cause analysis |
| Environment | Secure and structured | Intentionally calming with reduced triggers |
When someone is diagnosed with dementia, it can be a difficult and emotional experience for both the individual and their family. As a loved one’s cognitive decline progresses, they may exhibit unexpected behaviors—physical or verbal aggression, paranoia, severe mood swings, or profound depression. Approximately 35% of dementia patients display frequent aggression, and up to 97% of community-dwelling individuals with dementia will develop behavioral and psychological symptoms at some point. These behaviors are often a form of communication, signaling unmet needs like pain, fear, frustration, or discomfort.
The challenge intensifies when behavioral symptoms occur. Many families find themselves overwhelmed, struggling to manage caregiving demands at home while watching their loved one’s quality of life decline. Traditional memory care facilities may not be equipped to handle residents with complex behavioral health needs, leaving families searching for a more comprehensive solution.
This is where behavioral memory care steps in. It goes beyond basic supervision and assistance with daily tasks. It provides a calm, structured, and secure environment staffed by caregivers trained in managing behaviors related to conditions like schizoaffective disorder, depressive episodes, PTSD, and anxiety. The goal is not just to manage symptoms, but to improve each resident’s dignity, comfort, and sense of purpose through individualized care plans, therapeutic activities, and non-pharmacological interventions.
I’m Jason Setsuda, a Board Certified Emergency Medicine Physician and CFO of Memory Lane Assisted Living, with over 10 years of experience in medicine and 5 years in medical administration. Throughout my career, I’ve seen how effective behavioral memory care transforms lives by addressing both the cognitive and emotional complexities of dementia. In this guide, I’ll walk you through what behavioral memory care truly means, who it’s designed for, how it works, and how to find the right community for your loved one.
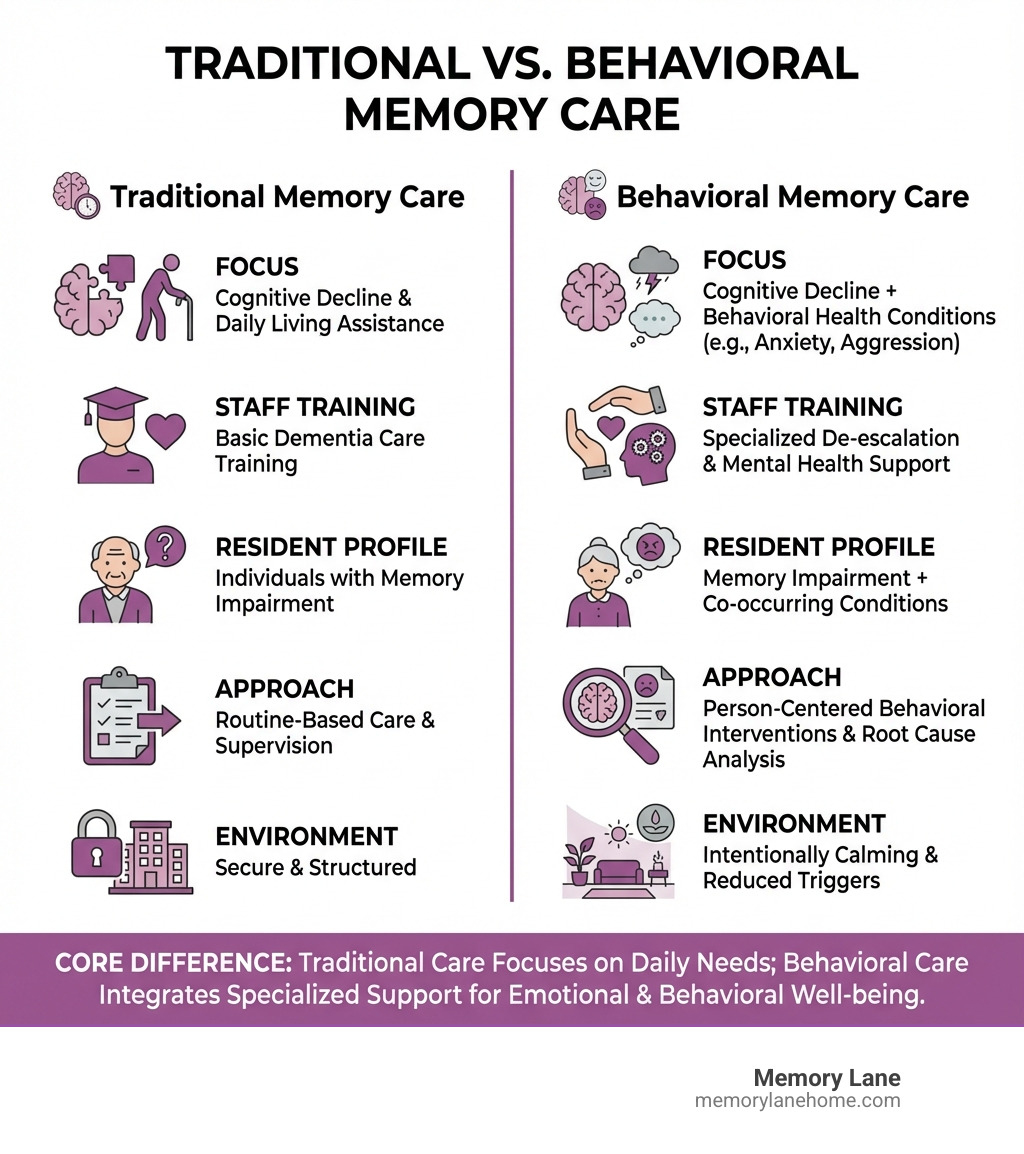
This infographic shows the differences between traditional memory care (focused on cognitive support and daily living assistance) and behavioral memory care (which adds specialized behavioral health support, trained staff in de-escalation techniques, personalized interventions for triggers, secure calming environments, and integrated treatment for co-occurring mental health conditions like anxiety, depression, and PTSD).
Easy behavioral memory care glossary:
Understanding Behavioral Memory Care: A Deeper Level of Support
At Memory Lane, we understand that caring for a loved one with memory impairment is a unique and challenging experience. When you layer on a behavioral health concern, the challenges can become even more complex and demanding. Behavioral memory care is a specialized approach that goes beyond the services offered in traditional memory care. It focuses on integrating strategies that support residents’ behavioral and emotional well-being alongside their cognitive and physical health. This person-centered approach acknowledges that challenging behaviors often stem from unmet needs or difficulties in communication, aiming to understand and address the root causes.
Our goal is to create a calm, structured, and secure environment, with trained staff, therapeutic programming, and personalized routines that help residents feel safe, understood, and empowered. This specialized care is designed to offer a holistic approach, supporting emotional well-being along with cognitive and physical health.
Who is Behavioral Memory Care Designed For?
Behavioral memory care is ideal for individuals experiencing significant memory impairment due to various forms of dementia, especially when these conditions are accompanied by co-existing behavioral health diagnoses. These conditions often include:
- Alzheimer’s disease: The most common form of dementia, accounting for 60-80% of cases, which progressively impacts memory, thinking, and behavior.
- Vascular dementia: Often caused by reduced blood flow to the brain due to strokes or other vascular conditions, affecting cognitive function.
- Lewy body dementia: Characterized by protein deposits in the brain that can affect both cognitive and physical abilities, often leading to visual hallucinations and fluctuations in alertness.
- Frontotemporal dementia: This type of dementia impacts the frontal and temporal lobes of the brain, leading to prominent changes in behavior, personality, and communication.
- Mixed dementia: A combination of two or more dementia types, often Alzheimer’s disease and vascular dementia.
Beyond the primary dementia diagnosis, behavioral memory care is specifically designed for individuals who also experience secondary behavioral health concerns such as anxiety, paranoia, depression, agitation, schizoaffective disorder, or PTSD. These conditions can significantly complicate care and often require a more specialized and integrated approach than traditional memory care provides.
Signs This Specialized Care Might Be the Right Fit
Recognizing when a loved one needs behavioral memory care can be challenging. It’s often a difficult decision, but understanding the signs can help families determine the best course of action for their loved one’s safety and well-being. Consider this specialized care if you observe any of the following:
- Increased aggression or agitation: Your loved one exhibits frequent outbursts, physical aggression, or persistent agitation that is difficult to manage at home. Approximately 35% of dementia patients display frequent aggression.
- Paranoia or delusions: Persistent false beliefs (e.g., someone is stealing from them, family members are imposters) or hallucinations that cause distress or safety concerns.
- Caregiver burnout: You, as a caregiver, are feeling overwhelmed, exhausted, or unable to cope with the demands of managing your loved one’s challenging behaviors.
- Safety concerns at home: There’s a risk of wandering, self-harm, or harm to others due to unpredictable behaviors. Wandering is a significant safety concern for many families.
- Difficulty with daily tasks: Increasing struggles with bathing, dressing, eating, or medication management, often accompanied by resistance or distress during these activities.
- Social withdrawal: A significant decline in social engagement and interaction, leading to increased isolation and potential worsening of mood.
- Information on early signs of dementia: While not always indicative of immediate behavioral care needs, early signs like memory loss affecting daily life, difficulty with familiar tasks, confusion with time or place, and changes in mood or personality can signal the need for professional assessment and potential future specialized care. Caring for a loved one with memory impairment is a unique and challenging experience.
The Core Components of Effective Behavioral Management
Effective behavioral memory care relies on a multi-faceted approach that prioritizes understanding the individual and their unique needs. It moves beyond simply reacting to behaviors and instead focuses on proactive strategies to prevent distress and promote well-being.
Our approach at Memory Lane is rooted in:
- Personalized care plans: Each resident receives a care plan custom to their cognitive challenges, behavioral triggers, medical history, and personal preferences. This ensures that care is responsive to their individual journey.
- Root cause analysis: We believe that behaviors are often a form of communication. Our staff are trained to investigate the underlying reasons for challenging behaviors, such as pain, hunger, discomfort, fear, or overstimulation, rather than just treating the symptom.
- De-escalation techniques: Our team is skilled in communication strategies designed to calm and reassure residents during moments of distress, preventing escalation of challenging behaviors.
- Non-pharmacological interventions: We prioritize non-medication-based approaches, recognizing that many behavioral issues can be managed effectively through environmental adjustments, meaningful activities, and empathetic interaction.
- DICE model: This clinical decision support tool helps our team systematically Describe the behavior, Investigate possible causes, Create a custom treatment plan (often non-pharmacological), and Evaluate outcomes.
- Unmet needs theory: This guiding principle suggests that most behavioral and psychological symptoms of dementia (BPSD) are expressions of unmet physical or psychosocial needs. Addressing these needs is central to our care philosophy.

The Importance of Specialized Staff Training in Behavioral Memory Care
The cornerstone of exceptional behavioral memory care is a highly trained and compassionate staff. Our team members undergo specialized training that goes far beyond general dementia care. This includes:
- Empathy-based communication: Learning to connect with residents on an emotional level, validating their feelings, and understanding their perspective, even when their perception of reality differs from ours.
- Managing aggression and agitation: Specific techniques for how to calm angry outbursts of people living with dementia and anxiety, focusing on redirection, reorientation, and creating a supportive stance. Over 45% of communities specifically train staff to handle and manage anxiety, aggression, and agitation, and about 90% use redirection and reorientation techniques.
- Validation therapy: A communication technique that acknowledges and respects the reality and personal truth of the person with dementia, rather than correcting them.
- Continuous education: Our staff regularly participate in ongoing training to stay updated on the latest research and best practices in dementia and behavioral health. Over 75% of memory care communities require specialized memory care training for staff, and we are proud to exceed this standard.
Designing a Supportive Physical Environment
The physical environment plays a critical role in minimizing behavioral challenges and promoting well-being in behavioral memory care. Our communities are intentionally designed to be both secure and calming, reducing potential triggers for agitation or confusion. Key environmental features include:
- Secure communities: Controlled access points and secured perimeters prevent wandering and ensure residents’ safety, offering sheltered freedom within our premises.
- Calming layouts: Easy-to-steer floor plans, clear signage, and consistent visual cues help residents orient themselves and reduce frustration.
- Sensory considerations: We minimize disturbing cues like harsh lighting, loud noises, and confusing reflections. Dimmers and full-spectrum light bulbs are preferred over harsh lighting.
- Memory boxes: Individualized display cases outside resident rooms, filled with personal items and photographs, help residents recognize their space and provide a sense of familiarity.
- Safe outdoor spaces: Enclosed courtyards and gardens provide secure opportunities for residents to enjoy fresh air, engage with nature, and exercise, which can significantly boost happiness and reduce agitation.
Strategies for Managing Challenging Behaviors
Managing challenging behaviors like aggression, paranoia, and depression requires patience, understanding, and a custom approach. Our team employs various strategies:
- Understanding triggers: We carefully observe residents to identify patterns and triggers for specific behaviors. For instance, aggression can stem from confusion, frustration, pain, or discomfort.
- Aggression management: Our staff use calm, reassuring communication, redirection to preferred activities, and empathetic validation of feelings. Physical restraint is avoided unless there is an imminent threat of danger.
- Addressing paranoia: When a resident experiences paranoia or delusions (like Capgras syndrome, where they believe a loved one is an imposter), we acknowledge their experience without arguing, offering reassurance and gently redirecting their focus. Hearing a podcast from NPR’s Radiolab program about Capgras Syndrome can offer insights into these complex experiences.
- Coping with depression: We focus on social engagement, meaningful activities, and a supportive environment to combat loneliness and apathy. Regular exercise and proper nutrition also play a vital role.
- Sundowning strategies: For residents who experience increased confusion and agitation in the late afternoon and evening (sundowning), we implement structured routines, manage lighting, and provide calming activities during these hours.
- Repetitive behaviors: These are often a way for residents to self-soothe or express an unmet need. We aim to understand the underlying cause and provide appropriate engagement or comfort.
- Using behavioral interventions in memory care: Our overarching philosophy is a “behavior-first” approach. This means we prioritize understanding and modifying the underlying trigger for a behavior rather than trying to control the behavior itself. This approach has been shown to reduce hospitalizations for dementia patients by more than three times the rate of older adults without cognitive impairment, and can prevent escalation to higher levels of care.
Therapeutic Engagement: Activities and Therapies that Improve Well-being
Beyond daily care, a vibrant program of therapeutic activities and engagement is fundamental to behavioral memory care. These activities are carefully chosen to stimulate cognitive abilities, foster joy, and maintain residents’ existing skills and independence. We believe that purposeful engagement is key to enhancing quality of life.
Beneficial Therapies in Behavioral Memory Care
At Memory Lane, we incorporate a variety of therapies custom to individual preferences and abilities:
- Music therapy: Can evoke powerful memories, reduce anxiety, and improve mood. Residents often respond positively to familiar songs, leading to increased social interaction and decreased agitation.
- Art therapy: Provides a creative outlet for self-expression, reduces stress, and can improve fine motor skills.
- Aromatherapy: The use of essential oils, such as lavender, has been shown to reduce behavioral issues like aggression and agitation in dementia patients. Evaluating the effects of diffused lavender in an adult day care center for patients with dementia in an effort to decrease behavioral issues: a pilot study suggests its potential benefits.
- Pet therapy: Interacting with animals can provide comfort, reduce loneliness, and stimulate social interaction. We also use robotic companion pets to offer comfort and companionship, especially for those in later stages of dementia. Consider a robotic stuffed animal as a source of comfort.
- Reminiscence therapy: Engaging residents in discussions about past events, using photos, music, or familiar objects, can validate their life experiences and foster a sense of identity and connection.
- Low-impact physical exercises: Activities like walking, gentle stretching, or chair exercises improve mood, sleep, and overall physical health, contributing to a reduction in challenging behaviors.
The Role of Medical Intervention and Medication
While behavioral memory care prioritizes non-pharmacological interventions, we understand that medical intervention and medication may sometimes be appropriate and necessary. Our approach is always cautious and collaborative, ensuring that medications are used as a last resort and with careful consideration.
- Last resort approach: We aim to exhaust all non-pharmacological strategies before considering medication. Experts suggest that 9 out of 10 times, dementia patients don’t need to be medicated with good care planning and productive activities.
- When medication is appropriate: Medication may be considered when behaviors pose a significant risk to the resident or others, or when non-pharmacological methods have proven ineffective and the resident is experiencing severe distress. This includes severe agitation, aggression, or psychosis.
- Antipsychotic risks: We are highly aware of the risks associated with antipsychotic medications in elderly patients with dementia, including increased mortality and adverse effects. Antipsychotic use in dementia: a systematic review of benefits and risks from meta-analyses highlights these concerns. Our medical director and care team carefully weigh the benefits against these risks.
- Collaboration with geriatric specialists: We work closely with geriatric psychiatrists and other medical professionals to ensure appropriate diagnosis and medication management. Telehealth visits can connect residents with these specialists, increasing availability.
- Regular medication reviews: All residents’ medications are regularly reviewed to ensure they are still necessary, effective, and not causing adverse side effects. Efforts are made to taper and discontinue antipsychotics periodically.
- Balancing benefits and side effects: For conditions like agitation, SSRIs (selective serotonin reuptake inhibitors) like citalopram may be considered, as studies like the Effect of citalopram on agitation in Alzheimer disease have explored their use. For apathy, medications like methylphenidate can be considered to improve motivation and function, as discussed in Pharmacological interventions for apathy in Alzheimer’s disease. Our goal is always to find the safest and most effective balance for each individual.
Understanding and managing Behavioral and Psychological Symptoms in Dementia is complex, and our team is dedicated to providing comprehensive, individualized care.
Navigating the Journey: Finding and Funding Your Loved One’s Care
Finding the right behavioral memory care community is a significant step, and we are here to support families throughout this journey. Our ultimate goal is to improve the quality of life for residents and provide peace of mind for their families. Knowing that your loved one is in a secure, supportive environment with specialized care can significantly alleviate the burden and stress of caregiving.
Options for Paying for Care
The cost of behavioral memory care can be a concern for many families. It’s important to explore all available options:
- Private pay: Many families initially cover costs through personal savings, pensions, or long-term care insurance.
- Long-term care insurance: If your loved one has a long-term care insurance policy, it may cover a portion of memory care expenses.
- Medicare limitations: Medicare generally does not cover long-term custodial care, including most memory care services. It primarily covers short-term skilled nursing care or specific medical treatments.
- Medicaid waivers: Medicaid is a state and federal program that can help with long-term care costs for eligible individuals with low income and assets. Michigan offers various Medicaid waiver programs that may cover assisted living or memory care services.
- Veterans benefits: Qualified veterans and their spouses may be eligible for Aid & Attendance benefits, which can help offset the cost of long-term care.
- Using the Eldercare Locator: This free public service connects you to services in your community, including information on payment options. You can also use tools like BenefitsCheckUp and Benefits.gov to find federal and state benefit programs that may assist with costs. Additionally, the Program of All-Inclusive Care for the Elderly (PACE) may be an option for some individuals. For general information on long-term care, LongTermCare.gov is a valuable resource.
How to Find the Right Community
Choosing the right behavioral memory care community in Michigan for your loved one involves careful research and consideration. We recommend the following steps:
- Assessing care needs: Start by thoroughly evaluating your loved one’s specific needs, including the nature and severity of their cognitive and behavioral challenges.
- Touring facilities: Visit several communities in Ann Arbor, Ypsilanti, Saline, or other Michigan locations that specialize in behavioral memory care. Pay attention to the atmosphere, staff interactions, and resident engagement.
- Observing staff interactions: During tours, observe how staff members interact with residents. Do they seem patient, compassionate, and engaged? Do they use specialized communication techniques?
- Reviewing state licenses and regulations: Ensure the community is properly licensed and adheres to all state regulations for memory care facilities in Michigan.
- Talking to other families: If possible, speak with families of current residents to get their perspective on the care provided and their experience with the community.
- Consulting your local Area Agency on Aging: These agencies can provide valuable resources and guidance on local memory care options and support services in Michigan.
- Connecting with advocacy groups: Organizations like the Alzheimer’s Association (which also has local chapters in Michigan), the Alzheimer’s Foundation of America, the Lewy Body Dementia Association, and the Association for Frontotemporal Degeneration can offer support, information, and help you find resources. The Eldercare Locator is another excellent starting point for finding local services.
Here are some questions we encourage families to ask when touring a potential community:
- What is your staff-to-resident ratio, especially during evening and overnight hours?
- What specialized training do your staff receive in managing challenging behaviors?
- How do you personalize care plans, and how often are they reviewed?
- What non-pharmacological interventions do you use for aggression, paranoia, or agitation?
- How is the physical environment designed to support residents with behavioral challenges?
- What therapeutic activities and programs are offered, and how are they custom to individual needs?
- What is your policy regarding medical intervention and medication for behavioral symptoms?
- How do you communicate with families about their loved one’s progress and any changes in their care plan?
Frequently Asked Questions about Behavioral Memory Care
What causes aggression and other challenging behaviors in dementia?
Challenging behaviors in dementia are rarely intentional. Instead, they are often a form of communication, signaling unmet needs or distress. Common causes include:
- Communication of unmet needs: The inability to express pain, hunger, thirst, or the need to use the restroom.
- Pain or discomfort: Untreated physical pain (e.g., arthritis, dental issues) or discomfort from a medical condition like a urinary tract infection (UTI) or constipation. Pain is present in 46% to 56% of patients with dementia, but only 20% to 40% receive analgesics.
- Fear and confusion: Disorientation, memory loss, and difficulty understanding their surroundings can lead to anxiety and fear.
- Frustration: Inability to perform familiar tasks or communicate effectively can lead to intense frustration.
- Environmental triggers: Overstimulation (loud noises, bright lights, large crowds), unfamiliar environments, or even confusing reflections can trigger agitation.
- Side effects of medication: Some medications can cause side effects that mimic or worsen behavioral symptoms.
Can a memory care facility evict a resident for aggressive behavior?
While rare, a memory care facility may, as a last resort, evict a resident for aggressive behavior if it poses a persistent danger to themselves or others, or if the behavior is spontaneously aggressive and cannot be safely managed. Our goal at Memory Lane is always to manage and mitigate challenging behaviors through specialized care plans and interventions. Eviction is typically a final step after all other behavioral management strategies and interventions have been exhausted, and usually involves clear contractual agreements and adherence to state regulations. We work closely with families to explore all possible solutions before such a decision is considered.
How does behavioral memory care improve a resident’s quality of life?
Behavioral memory care significantly improves a resident’s quality of life by:
- Reduces agitation and stress: By identifying and addressing the root causes of distress, we create a calmer, more predictable environment.
- Fosters connection and purpose: Personalized activities and social engagement help residents feel valued and connected, combating isolation.
- Builds confidence: Supporting residents in maintaining their abilities and providing opportunities for success boosts their self-esteem.
- Provides a safe and predictable environment: A secure setting reduces fear and confusion, allowing residents to feel safe and at ease.
- Supports independence: Our person-centered approach encourages residents to do as much as they can for themselves, preserving their autonomy.
Memory care enriches the lives of its residents by providing specialized support that allows them to thrive despite the challenges of dementia, offering a dignified and fulfilling lifestyle.
Conclusion
Behavioral memory care represents a crucial evolution in dementia care, offering a specialized solution for individuals facing complex behavioral and cognitive challenges. It’s a holistic and compassionate approach that prioritizes understanding the person behind the diagnosis, addressing their unmet needs, and enriching their daily lives through purposeful engagement and a supportive environment. The benefits extend not only to the residents, who experience improved well-being and dignity, but also to their families, who gain invaluable peace of mind knowing their loved one is receiving the highest level of specialized care.
At Memory Lane, we are dedicated to providing exceptional behavioral memory care in Michigan, with locations in Ann Arbor, Ypsilanti, and Saline. We create personalized care plans that honor each individual’s life story and needs, fostering an environment where every resident can feel safe, understood, and truly engaged.



