Does Medicaid Cover Nursing Home Care for Dementia 2025
The Financial Realities of Long-Term Dementia Care
Does Medicaid cover nursing home care for dementia? Yes, Medicaid covers 100% of nursing home costs for eligible individuals with dementia, including room, board, skilled nursing care, and specialized memory care services. This coverage is available in all 50 states and Washington D.C. as an entitlement program, meaning all who qualify will receive benefits.
Quick Answer: Medicaid Coverage for Dementia Nursing Home Care
- Full Coverage: Medicaid pays 100% of costs in certified nursing homes
- Services Included: Skilled nursing, personal care, medication management, therapies, meals, and 24/7 supervision
- Eligibility Required: Must meet both financial limits (typically $2,000 in assets) and medical necessity
- No Time Limit: Coverage continues as long as care is needed and eligibility is maintained
- Room & Board: Fully covered in nursing homes (unlike assisted living)
Finding long-term care for a loved one with dementia is emotionally and financially overwhelming. The lifetime cost of dementia care can exceed $390,000, with national costs projected at $360 billion for 2024. It’s no surprise that nearly two-thirds of nursing home residents rely on Medicaid.
The good news is that Medicaid is the primary funding source for nursing home care for people with dementia, covering the full cost for eligible individuals. Unlike Medicare’s limited 100-day coverage for skilled nursing, Medicaid provides long-term coverage for as long as needed.
However, navigating Medicaid’s complex, state-specific rules for eligibility, assets, and applications can be daunting, especially while juggling medical and family decisions.
I’m Jason Setsuda, a Board Certified Emergency Medicine Physician and CFO of Memory Lane Assisted Living. With over 15 years in healthcare administration, I’ve guided many families through the question of does Medicaid cover nursing home care for dementia. This guide will break down what Medicaid covers, how to qualify, and how to find the right care for your loved one.
Does medicaid cover nursing home care for dementia terminology:
Does Medicaid Cover Nursing Home Care for Dementia?
The short answer is a resounding yes! For eligible individuals in Michigan, Medicaid covers nursing home care for dementia. This is a crucial distinction, as many other programs, like Medicare, offer only limited or short-term coverage for long-term care.
Medicaid considers nursing homes as “institutional care communities.” In all states, including Michigan, Medicaid will pay for 100% of nursing home care for eligible adults with Alzheimer’s or another type of dementia. This is because institutional care is an entitlement designated by Medicaid, meaning this type of care will always be provided to Medicaid recipients who qualify. This full coverage includes the cost of room and board, health care services, personal care services, meals, and any memory care services provided within that setting.
This is especially vital given that almost two-thirds of nursing home residents are Medicaid beneficiaries. If your loved one requires the comprehensive, 24/7 care provided in a nursing home due to their dementia, Medicaid can step in where other resources fall short.
What Specific Dementia Care Services Does Medicaid Cover in Nursing Homes?
When your loved one is in a Medicaid-certified nursing home, the program generally covers a wide range of services essential for dementia care. These are designed to meet the resident’s physical, mental, and psychosocial needs.
Specific services often include:
- Skilled Nursing Care: 24/7 medical attention, including wound care and monitoring.
- Personal Care Assistance (ADLs): Help with daily tasks like bathing, dressing, eating, and mobility.
- Medication Management: Administration and oversight of all medications.
- Rehabilitative Services: Physical, occupational, and speech therapy to maintain function.
- Social and Dietary Services: Counseling, family support, and nutritionally balanced meals.
- 24-Hour Supervision: A secure environment to ensure safety and prevent wandering.
- Memory Care Services: Specialized programs and activities for cognitive engagement.
While Medicaid covers essential services, residents may be charged for non-essential, personal items such as a private room (unless medically necessary), in-room telephone/television, personal clothing, special grooming items, and social events beyond the facility’s standard program.
It’s always wise to ask for a detailed breakdown of what is included and what might incur additional costs when considering a facility.
How Medicaid Differs for Memory Care in Different Settings
Understanding how Medicaid covers memory care can be tricky because it varies depending on the care setting. While does Medicaid cover nursing home care for dementia is a clear “yes,” coverage for other settings is more nuanced.
Here’s a simplified comparison:
| Feature | Nursing Home (Institutional Care) | Assisted Living / Dedicated Memory Care Facilities (Community-Based) |
|---|---|---|
| Coverage Type | Institutional Medicaid (Entitlement) | Home and Community-Based Services (HCBS) Waivers (Optional) |
| Room & Board | Fully covered for eligible individuals | Generally NOT covered; residents pay privately |
| Medical/Care Services | Fully covered (skilled nursing, personal care, therapies, memory care) | Covered via waivers (personal care, therapies, memory care programs) |
| Availability | Guaranteed for eligible individuals in certified facilities | Limited spots, waiting lists common, varies by state |
| Level of Care Required | Typically higher, requiring skilled nursing or extensive personal care | Often for those needing assistance with ADLs but not 24/7 skilled care |
Home and Community-Based Services (HCBS) Waivers are special Medicaid programs that fund long-term services in settings like assisted living facilities or at home. These waivers are valuable for Michigan residents with dementia who don’t yet need intensive nursing home care.
However, HCBS waivers are not an entitlement; they have limited spots and potential waiting lists. Each state designs its own waivers, so covered services and eligibility vary. For instance, a waiver might cover personal care in assisted living, but the resident still pays for room and board.
We encourage families in Ann Arbor, Ypsilanti, and Saline, Michigan, to investigate the specific HCBS waivers available through the Michigan Department of Health and Human Services (MDHHS) to understand what options might be available for community-based memory care. You can find more information on HCBS programs directly from Medicaid’s website.
Qualifying for Medicaid: Navigating the Eligibility Maze
Understanding that does Medicaid cover nursing home care for dementia is only half the battle; the other half is qualifying for it. Medicaid is a state-run program, jointly funded by federal and state governments. This means while there are federal guidelines, each state, like Michigan, sets its own specific eligibility rules. We’ll explore the two main types of eligibility: financial and functional.

Financial Eligibility: Income and Asset Limits
Medicaid is a needs-based program, so financial eligibility is paramount. Your loved one must demonstrate limited income and assets to qualify.
- Income Limits: These vary by state. In Michigan, individuals applying for nursing home care must meet a specific income limit (e.g., the 2023 limit for many states was $2,742/month). Beneficiaries with income typically contribute a portion towards their care cost. Limits change annually, so check with the Michigan Department of Health and Human Services (MDHHS) for current figures.
- Asset Limits: Countable assets are generally limited to $2,000 for an individual. Exempt assets often include a primary home (up to a certain equity value), one vehicle, personal belongings, and pre-paid burial plans.
Medicaid Spend-Down: If your loved one’s income or assets exceed the limits, they may still qualify through a “spend-down” process. This involves using excess income or assets to pay for medical expenses until they reach the eligibility threshold. This is a complex area, and we strongly recommend consulting with an elder law attorney or Certified Medicaid Planner in Michigan.
Spousal Impoverishment Rules: Medicaid has specific guidelines to protect the “community spouse” (the spouse not requiring nursing home care) from becoming impoverished. These rules allow the community spouse to keep a certain amount of assets and a portion of the institutionalized spouse’s income. Again, these rules are state-specific for Michigan and require careful planning.
Functional Eligibility: Proving the Need for Care
Beyond financial requirements, your loved one must also demonstrate a medical need for nursing home care. This is known as meeting the Nursing Home Level of Care (NHLOC) criteria.
- Medical Necessity: A physician must certify the need for nursing home level care. This usually involves assessing the need for help with Activities of Daily Living (ADLs) like bathing and dressing, and Instrumental Activities of Daily Living (IADLs) like medication management.
- Cognitive Impairment Assessment: For dementia patients, the assessment evaluates cognitive decline. A challenge is that these assessments sometimes undervalue cognitive issues compared to physical ones, which can delay care access despite significant safety risks.
- Dementia Diagnosis: A formal diagnosis is critical. The assessment considers the dementia’s impact on daily function, behavior, and safety.
In Michigan, the MDHHS uses specific tools and criteria to determine NHLOC. It’s important that the assessment accurately reflects the comprehensive needs of a person with dementia, including supervision requirements, behavioral symptoms, and impaired decision-making abilities.
The Application Process and Finding a Facility
Once you understand the eligibility criteria, the next step is the application process and finding a suitable Medicaid-certified facility in Michigan.
How to Apply for Medicaid for Nursing Home Care
Applying for Medicaid can be a detailed process, but with careful preparation, it’s manageable.
- Contact Your State’s Medicaid Agency: For residents of Ann Arbor, Ypsilanti, or Saline, Michigan, your first step is to contact the Michigan Department of Health and Human Services (MDHHS). You can find contact information and resources on the Medicaid.gov website or directly through the MDHHS website.
- Gather Required Documents: Be prepared to provide extensive documentation, including proof of identity, residency, income, and assets. This means gathering Social Security cards, birth certificates, bank statements for the 60-month look-back period, property deeds, vehicle registrations, and all insurance policies. You will also need to document any asset transfers.
- Submit the Application: Depending on Michigan’s options, you may be able to apply online, by mail, or in person at a local MDHHS office.
- Cooperate with the Review Process: Medicaid officials will review your application and may request additional information. They will also conduct the functional assessment to determine NHLOC.
- Consider Professional Help: Given the complexity of Medicaid rules, especially regarding asset protection and the look-back period, many families find it beneficial to work with an Elder Law Attorney or a Certified Medicaid Planner in Michigan. These professionals can help ensure a smooth application process.
Finding a Medicaid-Certified Nursing Home or Memory Care Provider
Not all nursing homes or memory care facilities accept Medicaid. Those that do must be specifically licensed and certified as a Medicaid Nursing Facility (NF) by the state survey agency.
- Understand “Medicaid Beds”: A “Medicaid bed” refers to a bed in a skilled nursing facility designated for residents whose care is covered by Medicaid. While most nursing homes accept Medicaid, they may have a limited number of these beds.
- Use Available Resources:
- Medicare.gov: Visit Medicare.gov to search for and compare Medicare- and Medicaid-certified nursing homes in your area, including Ann Arbor, Ypsilanti, and Saline.
- Michigan MDHHS: The Michigan Department of Health and Human Services may provide lists of Medicaid-certified facilities.
- Area Agency on Aging: Your local Area Agency on Aging can be an excellent resource for finding facilities that work with Medicaid residents.
- Ask Providers Directly: When you contact facilities, ask key questions upfront:
- Is the facility Medicaid-certified and are “Medicaid beds” available for dementia care?
- What are the staffing ratios and what specific dementia training do staff receive?
- What activities and safety measures (e.g., for wandering) are in place for residents with cognitive impairments?
- Can you explain your resident rights policies?
At Memory Lane, we specialize in 24/7 personalized, compassionate support for individuals with dementia and Alzheimer’s. While we operate as an assisted living facility, we guide families through understanding all their options, including how Medicaid can play a role in long-term care planning.
Understanding Patient Rights and Ensuring Quality Care
Beyond the financial aspects, ensuring quality care and upholding the rights of your loved one with dementia is paramount. A dementia diagnosis does not diminish a person’s rights or their need for dignity and respect.
What Are the Rights of Dementia Patients Under Medicaid?
Dementia patients receiving nursing home care under Medicaid are protected by federal and state laws that guarantee specific rights. These include:
- Appropriate and Dignified Care: Care must be custom to their needs and delivered with respect.
- Participation in Care Planning: The right to be involved in creating their care plan.
- Freedom from Restraints: The right to be free from chemical or physical restraints used for convenience.
- Privacy and Financial Management: The right to privacy and to manage their own finances (unless legally represented).
- Freedom from Abuse and Neglect: A fundamental right to be safe from harm.
- Right to Voice Grievances: The ability to complain without fear of retaliation.
- Access to Information: The right to access their own medical records.
If you have concerns about your loved one’s rights or care, you can report them to the local Long-Term Care Ombudsman. In Michigan, the Ombudsman program advocates for residents of nursing homes and assisted living facilities.
How Can Families Ensure Quality of Care?
Ensuring a high quality of care for a loved one with dementia requires ongoing vigilance and active participation from families.
- Visit Regularly: Visit at various times to observe care and staff interactions.
- Communicate Openly: Build relationships with staff, ask questions, and share insights about your loved one.
- Participate in Care Planning: Attend meetings to ensure the care plan addresses specific dementia-related needs.
- Observe the Environment: Check for cleanliness, safety features, and proper maintenance.
- Advocate for Quality: Inquire about staff dementia training and use resources like your local Area Agency on Aging for support and guidance.
Other Funding Considerations for Dementia Care
While does Medicaid cover nursing home care for dementia is often the primary concern, Medicaid typically acts as a “payer of last resort.” This means that other payment sources must be exhausted first. Developing a comprehensive financial strategy often involves combining multiple resources.
Additional Public Benefits for Dementia Care
- Medicare: This federal program for those 65+ does not cover long-term custodial care. However, it may cover up to 100 days of skilled nursing care after a hospital stay, certain home health services, and cognitive assessments for dementia diagnosis.
- TRICARE & Veterans’ Benefits: TRICARE, for eligible military families, mirrors Medicare and generally doesn’t cover long-term custodial care. However, the Department of Veterans Affairs (VA) offers other significant benefits, like Aid and Attendance, which can help cover long-term care costs. We encourage eligible Michigan families to explore these VA benefits.
Standard health insurance policies generally do not cover long-term custodial care. Most coverage focuses on acute medical needs, not ongoing daily support.
Other Potential Resources
- Long-Term Care Insurance: If your loved one purchased a long-term care insurance policy, it could cover a significant portion of nursing home or assisted living costs. Review the policy carefully as details vary widely.
- Private Pay: Many families initially pay for care out-of-pocket using savings, investments, or proceeds from selling assets. This “spending down” of assets is often a step towards becoming Medicaid eligible.
- Community-Based Support Services: Before nursing home placement, explore local resources. Area Agencies on Aging and senior centers in Ann Arbor, Ypsilanti, and Saline, Michigan, may offer adult day care, respite care, or in-home support that can delay the need for institutional care.
- Veterans’ Benefits: Beyond TRICARE, the VA offers various programs that can help eligible veterans and their spouses with the costs of long-term care, including the Aid and Attendance Pension. This benefit can provide additional monthly income to help cover the costs of assisted living or nursing home care.
Frequently Asked Questions about Medicaid and Dementia Care
How long will Medicaid pay for nursing home care for dementia?
As long as an individual continues to meet Michigan’s financial and functional eligibility criteria, Medicaid will pay for their necessary nursing home care. Unlike Medicare’s 100-day limit for skilled nursing, Medicaid has no time limit for long-term custodial care, providing peace of mind for families facing progressive dementia.
Can Medicaid take my house if I go into a nursing home?
Medicaid’s Estate Recovery Program (MERP) allows states to seek reimbursement from a deceased beneficiary’s estate, which can include a home. However, significant protections exist. The home is typically exempt if a surviving spouse, a child under 21, or a blind or disabled child lives there. Other exemptions may apply. Since MERP rules vary by state, we strongly advise consulting an elder law attorney in Michigan to understand your specific situation and legal asset protection strategies.
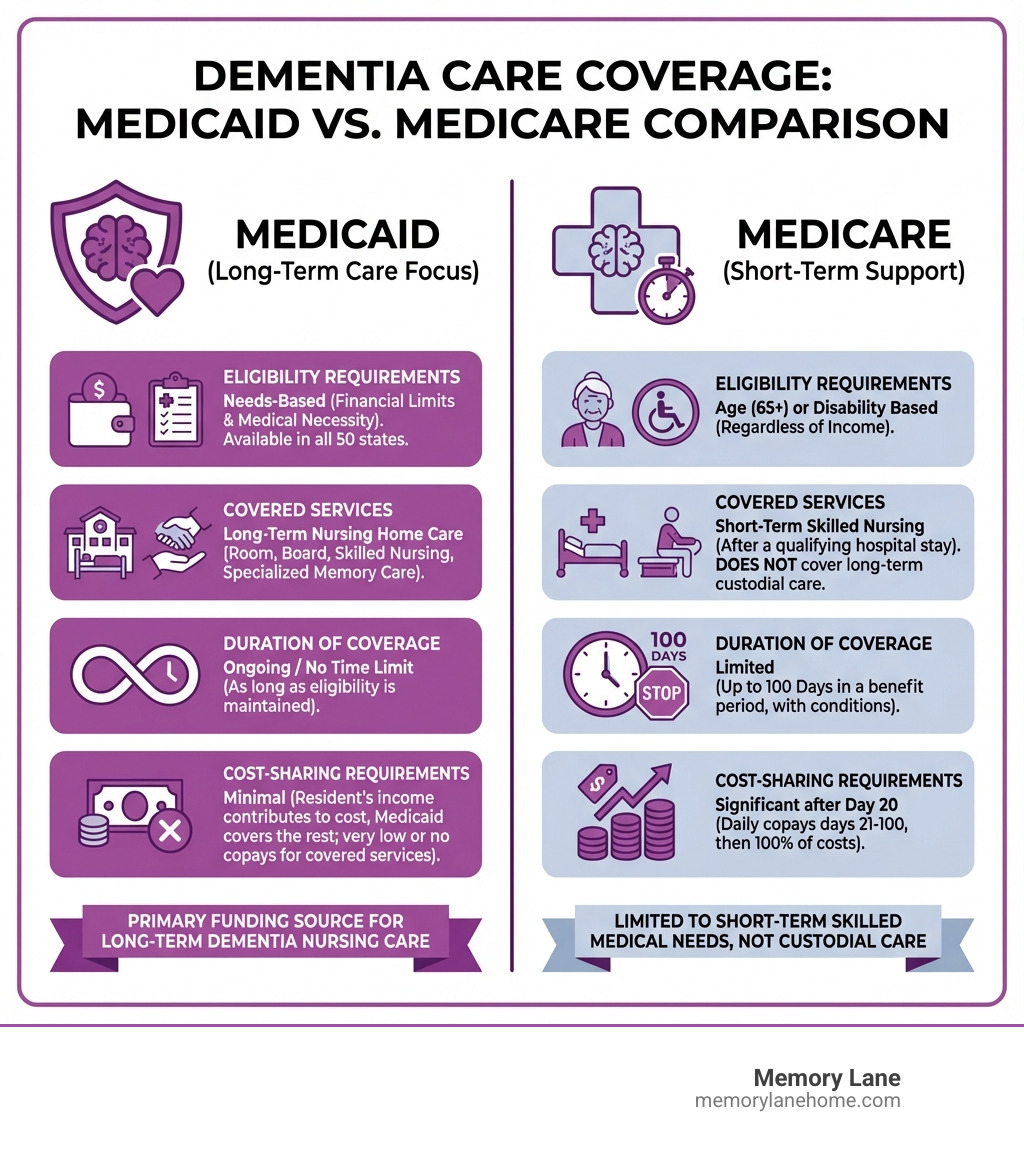
What is the difference between Medicare and Medicaid for dementia care?
Understanding the distinction between Medicare and Medicaid is crucial, as they serve different purposes for dementia care:
| Feature | Medicare | Medicaid |
|---|---|---|
| Purpose | Federal health insurance for those 65+ (or with certain disabilities) | Joint federal-state needs-based program for low-income individuals |
| Eligibility | Age (65+) or disability status | Income and asset limits (financial need) |
| Dementia Coverage | Short-term, skilled medical care; diagnostics, some therapies, 100 days skilled nursing post-hospitalization | Long-term custodial care (nursing homes), personal care, some community-based services |
| Room & Board | Not covered for long-term care | Covered in Medicaid-certified nursing homes; generally not in assisted living |
| Duration | Limited (e.g., 100 days for skilled nursing) | Indefinite, as long as eligibility is maintained |
In short, Medicare covers acute medical needs and short-term skilled care. Medicaid is the primary payer for long-term custodial care for those who meet financial and medical eligibility.
Conclusion: Taking the Next Step in Your Care Journey
Navigating dementia care is an emotional and financial challenge. We hope this guide has clarified Medicaid’s critical role as a safety net for covering nursing home care.
While the answer to does Medicaid cover nursing home care for dementia is yes, accessing it requires careful planning and a diligent application. Since rules vary, always consult Michigan’s Medicaid agency or a local elder law expert for personalized advice.
Early planning is key. Even if nursing home care isn’t immediately needed, understanding your options can alleviate significant stress. It’s a complex system, but with the right resources, navigating it is possible.
At Memory Lane, we understand the unique challenges families face when a loved one has dementia. We are committed to providing compassionate, specialized care that improves the quality of life and preserves the dignity of each resident. While we are a memory care assisted living facility, we are here to help you understand the full spectrum of care options and guide you toward the best solution for your family.
Explore our dementia care services to learn more about how we can support your loved one on their journey.

